Subscriber Benefit
As a subscriber you can listen to articles at work, in the car, or while you work out. Subscribe NowIt’s long been known that Obamacare would make health benefits more expensive for most employers.
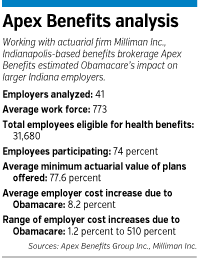
Now, it’s finally becoming clearer by how much: about 9 percent, on average, according to a series of actuarial studies of employers by benefits consulting firm Apex Benefits Group Inc. That punches out to $713 per worker for the 41 employers Apex studied.
 That financial impact isn’t large enough, by itself, to generate large-scale changes among employers, according to benefits brokers, although some companies will see their costs skyrocket and others, particularly small employers with older workers, might actually see costs decrease.
That financial impact isn’t large enough, by itself, to generate large-scale changes among employers, according to benefits brokers, although some companies will see their costs skyrocket and others, particularly small employers with older workers, might actually see costs decrease.
But combined with the annual faster-than-inflation rise in health benefits costs and Obamacare’s creation of a new option for employers—tax-subsidized individual insurance sold via online exchanges—the increased costs are prompting employers to consider major changes in the next few years.
“There’s a tipping point, where we’re seeing employers look at this stuff differently in terms of what they’re going to do longer term,” said John Gause, president of Indianapolis-based Apex Benefits. “Some employers aren’t just saying, ‘We can take this thing.’ Or, ‘We can accept the increase.’ They’re looking for opportunities.”
Already, many employers—such as Indiana University and numerous public school districts—have decided to hold their part-time workers to fewer than 30 hours a week, so they will not trip Obamacare’s requirement to provide coverage.
Some employers, including Indiana University and Centaur’s Hoosier Park and Indiana Grand racinos, are creating programs to help those part-timers navigate Obamacare’s exchanges, which have so far been inaccessible to most workers due to technical problems.
 Gause
GauseOther employers are going further, denying health coverage to workers’ spouses. That’s what Cincinnati-based Kroger Inc. announced in September. In other cases, employers are talking about outsourcing their low-wage or part-time workers to staffing firms so those workers have a better chance of qualifying for tax-subsidized health coverage on the exchanges.
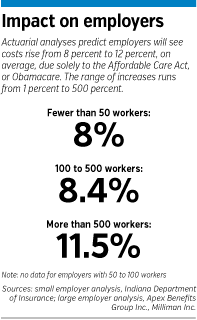
Apex, in partnership with the actuarial firm Milliman Inc., analyzed only employers with 100 or more workers. Apex’s finding of a 9.1-percent average increase jibes with a separate study by the Indiana Department of Insurance, which found that companies with fewer than 50 workers would see their benefits costs rise an average of 8 percent. That study, unlike the Apex study, included all new expenses small employers have incurred since Obamacare, formally known as the Affordable Care Act, became law in 2010.
Underlying both studies, however, is a huge range of potential outcomes for employers. The employers Apex studied face cost increases as low as 1 percent and as high as 510 percent. The high end applied to an employer that had to extend coverage to numerous workers who previously weren’t covered.
The Insurance Department’s study found that some employers with fewer than 50 workers, if their employees tend to be older or sicker, would even see their costs go down because of Obamacare.
The list of factors Apex considered in its study was long:
 Taxes: Obamacare funds its expansion of health insurance coverage by creating a variety of new taxes, which will fall on employers.
Taxes: Obamacare funds its expansion of health insurance coverage by creating a variety of new taxes, which will fall on employers.
• The transitional reinsurance fee of $5.25 per month for each person covered by an employer’s health plan will help insurers absorb the costs of no longer being able to deny coverage to sick individuals in the individual insurance market.
• A tax of $2 per health plan member to fund research into the cost-effectiveness of medical treatments.
• Taxes on the sales of medical devices and pharmaceuticals, which could raise the prices paid by employers’ medical plans for those products.
Benefit mandates: Obamacare requires all employers to cover contraception, mental health care and various other benefits. The majority of large-employer plans already covered all or nearly all these things, but the mandates add costs for a few employers.
Reporting requirements: Employers have new responsibilities for reporting information on their health plans to the federal government, to verify they are providing coverage that meets the benefits mandates, that covers a sufficiently high percentage of the expected medical claims of each employee, and that is affordable to employees. Obamacare defines affordable as single coverage that costs workers no more than 9.5 percent of their household incomes.
Provider cost-shifting: Separate from the Affordable Care Act, the federal government has reduced reimbursement to hospitals and doctors through the federal Medicare program for seniors. And now that baby boomers are retiring, a wave of patients who used to be covered by private insurance, which pays providers higher rates, is now moving into the lower-paying Medicare program.
Migration: Because Obamacare requires all individuals to obtain health insurance by Jan. 1, Apex’s analysis assumed that many employers would see a higher percentage of employees sign up for the employer-sponsored insurance. Having more people enrolled will mean an employer spends more on health benefits.
The participation rate for the companies in Apex’s study is currently 74 percent.
Also because of the individual mandate, Apex expects more employees will bring their children who are under age 26 onto their employer-sponsored coverage.
For some employers, this migration of new people onto their health plans will be helpful, if those new members are healthier. But if the influx of new members is generally sicker, an employer would pay more.
“As a result of the individual mandate, more employees are going to be accessing coverage through the employer, because in most of the cases it’s considered affordable,” said Tracey Gavin, leader of the health care reform practice at Apex.•
Please enable JavaScript to view this content.

Editor's note: You can comment on IBJ stories by signing in to your IBJ account. If you have not registered, please sign up for a free account now. Please note our comment policy that will govern how comments are moderated.