Subscriber Benefit
As a subscriber you can listen to articles at work, in the car, or while you work out. Subscribe NowObamacare was supposed to extend health insurance coverage to an additional 450,000 Hoosiers.
But what if it extends coverage to no one?
Less than two months before the bulk of Obamacare takes effect, that outcome is at least a possibility in Indiana.
Even though the Affordable Care Act, also known as Obamacare, will raise various taxes to subsidize the cost of expanding insurance coverage, Indiana might say no to all of its new funding, to the tune of $1.2 billion per year. That also means the state would say no to a reduction by more than half of the 810,000 Hoosiers that go without health insurance for a time each year.
 Pence
PenceInstead, Gov. Mike Pence has pursued policies that are, at least in part, designed to keep taxes and costs low for larger employers in Indiana.
There is a rationale for favoring larger employers, some economists say. But even conservative opponents of Obamacare said Pence’s policy is problematic both economically and politically.
The state will not expand eligibility for Medicaid by 2014, as the Pence administration continues to try to work out an alternative deal for expansion with the Obama administration. Meanwhile, about 182,000 Hoosiers who would likely have enrolled in Medicaid next year won’t be able to.
State officials also want to roll back Obamacare tax credits designed to help Hoosiers buy health insurance in an online marketplace called an exchange. In October, the state sued the Internal Revenue Service to invalidate those tax credits, saying Congress approved them only for state-run exchanges, not for the federal exchange that Indiana is part of.
 Zoeller
ZoellerThe lawsuit, filed by Indiana Attorney General Greg Zoeller, will take a while to play out. But if successful, it would disqualify an estimated 265,000 Hoosiers who would otherwise receive tax credits.
Under Obamacare, no employer can be fined for not providing health insurance unless one of its employees first obtains a tax credit to buy insurance through an insurance exchange. By blocking the tax credits, Indiana could block all penalties against employers.
“In short, by not creating an Exchange, the use of which may trigger financial penalties for employers, a State can create a more hospitable business environment for large employers,” Zoeller wrote in his lawsuit.
The Pence administration declared its support for the lawsuit when it was filed, but declined to comment for this story.
By large employers, Zoeller referred to companies with 50 or more workers. Companies with fewer workers are not required by Obamacare to provide health insurance.
There are some economic reasons for the Pence administration to favor large employers over smaller ones.
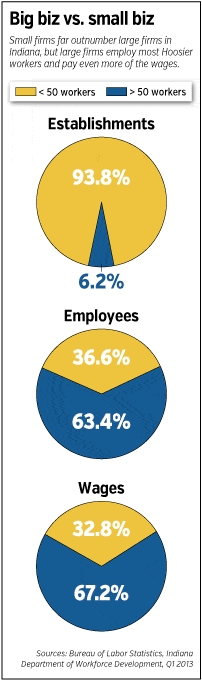
Businesses with 50 or more workers account for nearly two-thirds of all jobs in Indiana and even a bit more of the total wages paid.
In addition, large companies or large investors from out of state accounted for more than half the job growth during the last economic expansion, from 2003 to 2008, according to a study published last year by Indiana University economists.
“Clearly, Indiana is dependent upon investment originating outside the state to create jobs,” wrote IU economists Tim Slaper and Ryan Krause.
In addition, Slaper and Krause noted, Obamacare’s employer mandate and tax subsidies create disincentives for businesses to grow larger.
For example, a company with 49 employees that does not offer health insurance would, when it hired its 50th worker, be required to pay for coverage for all 50 of its workers—or at least pay a $2,000 penalty for each worker.
 “The effects on Indiana’s employment could be substantial,” wrote Slaper and Krauss. They figured that if Obamacare had been in effect from 2003 to 2008, Indiana would have added 15 percent fewer jobs than it did.
“The effects on Indiana’s employment could be substantial,” wrote Slaper and Krauss. They figured that if Obamacare had been in effect from 2003 to 2008, Indiana would have added 15 percent fewer jobs than it did.
Smaller firms pay price
But in spite of the contributions of larger, out-of-state employers, the other half of Indiana’s job growth came from in-state companies with fewer than 50 workers, noted Slaper and Krause.
“Startups are the source of new life in an economy,” Slaper wrote in an email.
Even conservative health economists found Indiana’s attempt to block Obamacare’s tax subsidies puzzling.
“It doesn’t make sense to do anything at the expense of small firms,” said Devon Herrick, a health economist at the National Center for Policy Analysis, a conservative think tank in Dallas. “If you inhibit their creation, I think the downstream effect will be that there are fewer jobs 10 years later.”
Matt Kleymeyer, who advises businesses and individuals on their best options for health insurance, said he’s already had interest from some entrepreneurs and startups about using the exchanges and the tax credits that come with them instead of having a company health plan.
“It gives a startup company the opportunity to recruit and retain a strong employee base, without having to compete against some of the larger, more established firms in their industry that offer really rich benefits,” said Kleymeyer, manager of Tennessee-based Bernard Health’s Indianapolis office.
The expansion of Medicaid would help some companies, especially those that have a significant number of low-wage workers.
The California-based Kaiser Family Foundation estimated that 62 percent of workers in Indiana’s service and agricultural companies are currently uninsured and would qualify for Medicaid if the state expanded eligibility for the program up to 138 percent of the federal poverty limit, as called for by Obamacare.
In a March analysis, Jackson Hewitt Tax Service estimated that, by not expanding Medicaid, Indiana employers could pay $37 million to $55 million in penalties for not providing health insurance.
But if Indiana neither expands Medicaid nor has tax subsidies available, no employers would incur any penalties for not offering health coverage.
Leaving money on the table
The savings to employers, however, would be dwarfed by the revenue Indiana would be giving up.
Kaiser estimates that 182,000 Hoosier adults with incomes below the federal poverty limit would sign up for Medicaid, and that the federal government would spend about $2,700, on average, for each of them. That totals $490 million per year.
Kaiser also calculated that 265,000 Hoosiers would qualify for a tax subsidy and actually buy health insurance in the Obamacare exchange by 2016. With those subsidies averaging nearly $2,700, that’s another $710 million.
Combined, that $1.2 billion in new revenue would provide less than a 1-percent boost to Indiana’s total personal income of $237 billion. And some of the new money would simply crowd out other money that’s now flowing into the state’s economy, said Herrick, the health economist.
But some argue that whatever money Indiana passes up would hurt hospitals and doctors and could, indirectly, come back to hurt employers, too, as hospitals and doctors continue to shift the cost of caring for the uninsured onto employers.
“We pay for it today; it’s just hidden,” said Brian Williams, a former aide to Gov. Evan Bayh and now a health care consultant for PricewaterhouseCoopers.
On Medicaid, Herrick supports Pence’s decision to hold out until he gets the OK to use the Healthy Indiana Plan as the vehicle for that expansion. HIP features health savings accounts and a cap on overall state spending—features the Obama administration has all but rejected.
However, Herrick added, if Indiana does succeed at nullifying the Obamacare subsidies, Pence and his fellow Republicans are likely to pay a political price.
“Can you imagine what would happen to a state politician if residents have to go and buy insurance that costs you $10,000, all the while being told by the opposing party, ‘You could have had a subsidy for $10,000,’?” Herrick said. “That is a strategy for getting defeated.”•
Please enable JavaScript to view this content.

Editor's note: You can comment on IBJ stories by signing in to your IBJ account. If you have not registered, please sign up for a free account now. Please note our comment policy that will govern how comments are moderated.