Subscriber Benefit
As a subscriber you can listen to articles at work, in the car, or while you work out. Subscribe NowWith Congress bringing back the idea of a government-run insurance plan, or public option, the debate is on again whether
there’s sufficient competition and choice in the health insurance market.
In Indianapolis, at least, that’s
becoming a harder case to make.
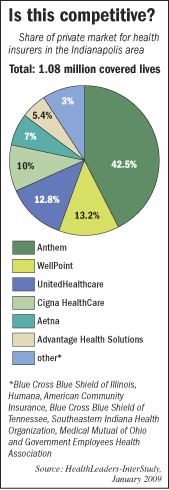
Anthem Blue Cross and Blue Shield continues to increase its market share in the
metro area, dwarfing its competitors. The Indianapolis-based company claimed 42.5 percent of the people covered by private
insurance this year, a big jump from its 35-percent stake last year, according to data from HealthLeaders-InterStudy, a Tennessee-based
market research firm.
The second-largest player is Minnesota-based UnitedHealthcare, with 12.8 percent of the
area’s customers.
 Vicki Perry, CEO of Advantage Health Solutions, sees vibrant competition in Indianapolis.
Vicki Perry, CEO of Advantage Health Solutions, sees vibrant competition in Indianapolis. United’s
stake in the market is actually smaller than that claimed by out-of-state insurance plans owned by Anthem’s parent company,
Indianapolis-based WellPoint Inc. Combined, those plans insure 13.2 percent of Indianapolis-area residents in private-funded
plans.
Duke Brown, owner of Duke’s Earth Service in Mooresville, said there is still some choice in health
insurance locally. The problem is, he said, competitors’ quotes on premiums are never more than about 10 percent apart.
“You’re picking the lesser of all evils,” Brown said. He has stomached premium increases for his
25-person firm of greater than 20 percent each of the last three years. So this year, he said, he’s likely going to
switch from Anthem to Minnesota-based Federated Insurance, which has recently been trying to grow in this area.
The experience has turned Brown, who describes his politics as “center-right,” to favor the public option.
But he said such a plan must come with reform of medical malpractice laws to keep enough doctors serving patients.
Indianapolis shows more market concentration than other cities, such as Cincinnati, according to Rick Byrne, an analyst
at HealthLeaders-InterStudy.
“Indianapolis is a bit unusual,” he said.
Nationally,
WellPoint is the largest private insurer. But it has substantial market share in only 14 states, so its share of the national
private insurance market last year was only about 14 percent, according to data from the company and the U.S. Census Bureau.
Statewide, Anthem’s commercial market share is slightly lower than in Indianapolis, about 38 percent, according
to figures from WellPoint.
Anti-trust issues
But Anthem’s increasing market
dominance here is bringing it some grief. In May, a union group called Central Indiana Jobs with Justice called on Indiana
Attorney General Greg Zoeller to investigate whether Indiana has a monopolistic market in health insurance.
The
group claimed WellPoint has 60-percent market share statewide, citing a study by the American Medical Association. The AMA
relied on data from HealthLeaders-InterStudy, but the two entities have since had a dispute about the AMA’s study.
The union group pointed out that the U.S. Department of Justice considers a market “highly concentrated”
when one firm has more than 42 percent market share.
“When just a couple of companies hold a near monopoly,
they not only set the prices, but they also make the rules and call the shots,” Allison Luthe, community organizer for
Central Indiana Jobs with Justice, said in a statement.
“It’s time for real comprehensive reform
that includes regulation and the choice of a public health insurance plan so we are no longer at the mercy of the private
health insurers in Indiana.”
Byrne, the HealthLeaders-InterStudy analyst, said the Indianapolis market
is on the threshold of becoming a monopoly market. If Anthem were able to pick up another big account, such as city and county
government employees, it could make the market significantly less competitive.
The city contracts are now held
by Indianapolis-based Advantage Health Solutions. Its CEO, Vicki Perry, however, still sees vibrant competition in the market.
“The greater their market share,” she said of Anthem, “the more interested the provider community
is that we have a good, long-term, local choice.”
That means doctors and hospitals are willing to give
Advantage attractive discounts on their prices, even though it brings them far fewer patients than Anthem.
“We
think this is a very exciting time for growth,” Perry added.
Anthem grew last year largely by adding customers
from M-Plan Inc., the local health maintenance organization, which ceased operation. Before it closed, the company held 10
percent of the Indianapolis-area market, according to HealthLeaders-InterStudy.
M-Plan recommended Anthem to
its 130,000 customers—and 85 percent of them chose Anthem. That included the state employees that had M-Plan insurance.
“Many of those organizations already had Anthem [among their insurance options] before M-Plan decided to exit
the market. We already had a relationship,” said Rob Hillman, president of Anthem in Indiana.
Hillman said
the Indianapolis market is still very competitive. He noted that when Anthem makes a bid for new business, it wins the client
only one out of five times.
“It’s a pretty fierce competition in the Indiana marketplace,”
Hillman said.
Anthem’s key point of competition is its network of doctors and hospitals. It has more doctors
and hospitals who have agreed to give discounts to Anthem members than to any other insurer in the state.
And
because Anthem has more patients in its plans than any other insurer, it can usually demand bigger discounts from doctors
and hospitals than can any other insurer.
That, of course, wins Anthem few fans among hospitals and, especially,
doctors. The Indiana State Medical Association helped sponsor legislation approved by the General Assembly in 2007 that forbids
Anthem from including clauses in its contracts that required doctors and hospitals to give it the largest discounts.
This past year, the ISMA backed a bill that would have allowed doctors and hospitals to cap the number of Anthem patients
they accept. It went nowhere.
Now that WellPoint and its peers are facing the prospect of much stricter regulations
from Congress, some doctors and hospitals are delighted.
“The insurance companies have been the robber
barons of the last decade,” said Dr. Pete Sallay, an orthopedic surgeon at Methodist Sports Medicine/The Orthopedic
Specialists. “They’re squealing right now. They need to squeal.”
Impact of reform
It’s not clear, however, that the health reforms being considered by Congress would do much to change
the market share of the biggest insurers—at least in the long term.
Shellie Stoddard, a credit analyst
at Standard & Poor’s in New York, said she would expect some small players to enter the market to take advantage
of the $450 billion in subsidies Congress plans to give low-income Americans to help them buy private insurance.
That’s what happened after Congress created the Medicare Part D prescription drug plan in 2003. But eventually, those
early entrants were bought up by larger companies, with relatively little impact on market shares.
Investors
in publicly traded health insurers fear that the public option would steal loads of customers away from their plans. Health
insurers’ stock prices have trended down since health reform started picking up steam this month.
But Les
Funtleyder, a health care stock analyst at Miller & Tabak & Co. in New York, said a government-run health plan will
have a hard time building up a network of hospitals and doctors to rival those of companies like WellPoint. The plan won’t
be able to pay doctors and hospitals too well, he said, if it also hopes to keep premiums low enough to attract customers.
“It looks like just an interesting form of Medicaid, which is attractive if you don’t have insurance,
but isn’t so attractive if you have access to insurance,” Funtleyder said. He added, “I don’t believe
it will shift the market share.”
What could have a bigger impact, said Advantage’s Perry, are the
market restrictions Congress plans to place on health insurers.
For example, it calls for health exchanges that
have only four plan designs. If those four levels permeate the entire market, it could hurt small companies like hers that
thrive on tailoring their plans to meet clients’ needs.
“Advantage feels it’s competitive because
we aren’t the typical insurance plan,” she said. “We really focus on longer-term solutions and patient engagement
and a lot of emphasis on wellness without costing the company a lot of money. I’m fearful if we only have one or two
options.”•
Please enable JavaScript to view this content.

Editor's note: You can comment on IBJ stories by signing in to your IBJ account. If you have not registered, please sign up for a free account now. Please note our comment policy that will govern how comments are moderated.