Subscriber Benefit
As a subscriber you can listen to articles at work, in the car, or while you work out. Subscribe NowEmployer activism is on the rise when it comes to keeping hospitals honest in their negotiations with health insurers.
Executives at Indianapolis-based WellPoint say groups of employers are increasingly airing their displeasure when
hospital systems ask for double-digit reimbursement increases.
 Goulet
Goulet“In many of our more difficult negotiations,
they’ve been more willing over the last year to participate as a local employer group, in getting involved and giving
their opinions in our negotiations with our facilities,” Ken Goulet, WellPoint’s CEO of commercial business, told
Wall Street analysts Jan. 27.
One public example came last year in Louisville, where an employer group stirred
up a negotiation involving WellPoint’s Anthem Blue Cross and Blue Shield subsidiary. The Louisville-Kentucky Business
Coalition on Health publicized that a local hospital system, Norton Healthcare, wanted a 27-percent reimbursement hike for
its children’s hospital.
The coalition then worked to form a network of health care providers that excluded
Norton. The plan is modeled on a Milwaukee program that requires hospitals to bid against one another to provide care to the
plan’s employer members. That plan has held costs steady since 2005.
Such is not the case for WellPoint
across the country. The cost of medical care for the 33 million people covered by its health plans rose nearly 9 percent last
year, after running at less than 8-percent increases for three straight years.
For hospital inpatient visits,
90 percent of the rise came from price hikes by health care providers.
Indiana has yet to see employer groups
take action as in Louisville or Milwaukee, and two Indianapolis groups focused on health say they have no plans to do so.
But companies do, in private, push back against their local hospitals, particularly in communities outside of Indianapolis.
Two prominent examples are Chrysler Corp. in Kokomo and Cummins Inc. in Columbus.
“Larger employers
that are more savvy are realizing that there’s a [provider] network component to their claims. They do want to have
more of a say,” said Rod Reasen, CEO of Mavum Consulting, a benefits brokerage in Indianapolis. “It’s happening
more now than it was in the past because employers are being pushed from every perspective.”
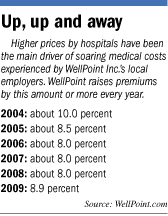
WellPoint raises its
premiums at least as fast as its medical costs rise, and typically more. Company executives reiterate
that point to investors in every quarterly conference call about its profits.
It’s
no wonder, then, that employers nationally have watched their premiums rise 131 percent in the past decade,
more than quadruple the rate of inflation. Even in 2009, when inflation was less than 1 percent, health
insurance premiums still rose 5 percent, according to an annual survey by the Kaiser Family Foundation.
WellPoint’s
Goulet said that cost trend, combined with the poor economy, has more employers than ever looking for
cost savings from WellPoint. Some employer groups, such as the Louisville coalition, are looking to build new insurance
plans that include only health care providers that agree to favorable pricing.
In addition, more employers than
ever last year signed up for WellPoint’s integrated health programs, which try to use preventive care and disease management
to change the health behaviors of the people covered by its plans.
WellPoint officials declined to cite any specific
Indiana example where an employer or employer group had injected its thoughts into a negotiation. But trying to appeal to
employers is one of the oldest tricks in the negotiating playbook—for both insurers and hospitals.
“This
game is what it is,” said Dave Shove, a health insurance analyst at BMO Capital Markets in New York. “The negotiations
take place in privacy until the 11th hour and then between 11 o’clock and midnight, both sides go public.”
That’s what recently occurred when contract talks soured between WellPoint’s Anthem subsidiary and Sisters
of St. Francis Health Services Inc., which operates 10 hospitals in Indiana, three of them in Indianapolis.
St.
Francis declared Anthem in breach of its contract in October 2008, and both sides quickly fired off letters to employers,
making their respective cases.
Anthem said St. Francis wanted an increase in reimbursement rates that would total
50 percent over a 39-month period, raising costs $80 million.
St. Francis said it simply wanted payments equal
to the going rates for hospitals in its marketplaces.
In an October 2008 interview, Anthem spokesman Tony Felts
specifically cited self-insured employers as a reason Anthem refused St. Francis’ demands.
“A 50-percent
reimbursement increase for Anthem gets passed on to those employers and their employees,” he said. “In this economic
climate, it’s just not acceptable.”
Doug Leonard, president of the Indiana Hospital Association,
said the rules of the American health care system give neither hospitals nor insurers much incentive to hold down costs.
The federal Medicare program, the largest insurance plan in the nation, pays hospitals for higher volumes and for
installing newer, more expensive equipment. So hospitals keep doing more stuff and adding new machines, Leonard said.
And the health insurance market rewards WellPoint—not so much for keeping prices low in absolute terms—but
for keeping its prices lower than any of its competitors.
Because WellPoint’s Anthem Blue Cross and Blue
Shield subsidiaries have commanding market shares in their 14 states, WellPoint typically gets a better price than any other
insurer. Even if that price is 9 percent higher than before, WellPoint knows its employer customers won’t find a better
deal anywhere else.
“The system simply rewards hospitals for bringing in more revenue. Anthem’s system
just rewards them for charging more than their costs,” Leonard said. “It’s frustrating because you’re
in this moral conflict all the time.”
For that reason, some of the key Indiana employer groups focused
on health care in Indiana said it’s unlikely they’ll follow the lead of the Louisville coalition. They’re
focusing, they say, on deeper issues.
The Employers Forum of Indiana helped create a program, Quality Health
First, that generates quality reports for doctors’ groups. WellPoint and its rival UnitedHealthcare have both agreed
to pay bonuses to the best-performing doctors on those reports.
Dr. Ned Lamkin, president of the Indiana Employers
Quality Health Alliance, said the work of his coalition and its national parent organization is aimed at changing the way
insurers pay hospitals for their services, not choosing sides in their battles.
In an e-mail, Lamkin wrote, “The
coalition movement is more focused on fundamental change and reform than entering into arguments under the existing arrangements.”•
Please enable JavaScript to view this content.

Editor's note: You can comment on IBJ stories by signing in to your IBJ account. If you have not registered, please sign up for a free account now. Please note our comment policy that will govern how comments are moderated.