Subscriber Benefit
As a subscriber you can listen to articles at work, in the car, or while you work out. Subscribe NowAt least there’s one positive thing that can be said about the sluggish economy: It put a temporary stop to the nursing shortage.
Most area hospitals report lower-than-normal vacancy rates, saying that some nurses have decided to put off retirement. Others who had left the profession have returned because their spouse lost their job, or because their retirement nest egg had shrunk by an unacceptable amount.
Lee Ann Blue, chief nursing officer at Wishard Health Services, said she’s seen a “historic” low vacancy rate and low turnover, as well.
“We have a pretty well-known ER and burn center and OB department, and there’s a waiting line for people to work there,” she said. “I believe the economy has played a role in that. I see less movement of nurses.”
She’s also seen, since 2008, more nurses who worked part time going full time.
“Right now, it’s a very good time from my perspective,” she said. “I’ve got people to take care of my patients.”
But administrators and nursing educators say it’s only a matter of time before a multi-sided whammy hits. When the economy improves, a wave of nurses will quit or retire. So will nursing faculty members, which means fewer teachers available to train new nurses—many of whom will need bachelor’s degrees or better to handle the increased demands and expectations they will face.
And if health care reform takes effect as written, there will be an estimated 30 million new people with insurance, straining the system even further. (How many of them will be in Indiana is uncertain.)
The Indiana Department of Workforce Development ranks nursing No. 5 on its list of in-demand jobs, projecting the need for more than 12,000 additional nurses by 2018.
At the same time, a study by worldwide recruiting firm Bernard Hodes Group found that 55 percent of nurses surveyed nationally expect to retire between 2011 and 2020. And a 2010 survey of schools indicates that 61 percent of the full-time nursing faculty in Indiana will be eligible to retire by 2017, according to Betsy Lee, director of the Indiana Patient Safety Center.
“All indications are we will have a very serious crisis when these people retire or go back to part time,” said Anita Siccardi, dean of nursing at Marian University.
Temporary spike
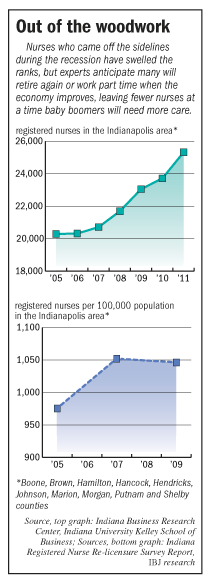
Retired and part-time nurses came out of the woodwork in 2008, the first full year of the recession, to supplement their incomes.
The Indianapolis metro area had held steady at 20,000 to 21,000 nurses from 2005 to 2007, but then began climbing—reaching 25,322 this year, according to the Indiana Business Research Center, an arm of the Kelley School of Business at Indiana University.
The ratio of nurses to the overall population in the Indianapolis area actually began swelling a year earlier. Studies by the Indiana Professional Licensing Agency show 1,052 nurses per 100,000 population in 2007 compared to 975.4 nurses in 2005.
The study, which is conducted every two years, shows the ratio leveling off in 2009. The 2011 study isn’t complete.
So what can be done to ensure enough nurses are on the job after the economy improves and many return to retirement or part-time status?
The simple answer would seem to be to train more nurses. And schools are trying. But many are stretched thin, with not enough faculty to keep up with the demand and budget restrictions that make it difficult to pay qualified teachers what they can earn in the field as nurses.
Marian University, which used to admit 50 nursing students a semester, now takes 64. At the University of Indianapolis, nursing Dean Anne Thomas said that last year, for the first time, the school enrolled clinical nursing students in its baccalaureate program in the fall as well as the spring.
“There’s a shortage of baccalaureate-prepared nurses who can go into community settings—because that’s not typically a place that associate-degree nurses work,” Thomas said. “We need people who have been educated to take care of ambiguous situations. When you go into somebody’s home, you’re in their home. You can’t make them do things. So you have to have people who are creative thinkers and can work with people from diverse backgrounds.”
Donna Boland, associate dean at the IU School of Nursing, said that school has “pretty much maxed out” capacity, “as have most established institutions in the state related to our resources.”
UIndy’s Siccardi has been in nursing for 50 years. She’s seen gluts and vacancies. But this time, she said, it’s different.
“This isn’t just simple supply and demand,” she said. “This is health care reform, this is the changes that have happened over the last maybe 20 years, that the community has not been hiring as many RNs. They’ve been hiring other types of people.”
When she broke her leg last year, Siccardi saw an emergency medical technician in the emergency room—not an ER nurse. She saw an athletic trainer in the orthopedic doctor’s office, not a nurse. And in her primary care office, a medical technician took her vital signs.
“For years, physicians and clinics and people in home health care have found they can do what they believe is a similar job with someone they can pay less money,” she said.
Rising demands
In the meantime, nurses are going to be called on to handle more complex cases. Doctors, nurses, educators and others point to a 2010 Institute of Medicine report called “The Future of Nursing,” which found that nurses’ roles, responsibilities and education need “to change significantly to meet the increased demand for care that will be created by health care reform and to advance improvements in America’s increasingly complex health system.”
The report said nurses should be fully engaged with other health professionals and assume leadership roles in redesigning care in the U.S. It called for residency training, increasing the percentage who attain a bachelor’s degree to 80 percent by 2020, and doubling the number who pursue doctorates.
Projections are that in the next eight years, 17 percent of nurses will work in hospitals, Siccardi said. The rest will go into the community—as public health nurses, in doctors’ offices and clinics, and in home health care.
“Hospitals aren’t making money because reimbursement isn’t what it used to be and technology is much more expensive,” she said. “So they’re looking at ways—wellness—to keep people out of the hospital.”
Collaborations
The other major shift in health care is an increase in collaborations. Darcy Burthay, chief nursing officer at St. Vincent Hospital, said schools and hospitals have been proactive in their partnerships, including a Marian University-St. Vincent Health collaboration to increase the number of nurses educated in central Indiana. The program, which began admitting students a year ago, incorporates online education and traditional clinical preparation.
The Indiana Patient Safety Center’s Lee said the new Indiana Center for Nursing was created in July through a merger of the Indiana Nursing Workforce Development Center, Nursing 2000 Central and Nursing 2000 North in response to “The Future of Nursing” report recommendation that there be more interprofessional collaboration, teamwork and education in health care. Its goal was to create one statewide nursing organization to prepare Indiana’s licensed nurses to meet the health care needs of Indiana’s citizens.
Also as part of “The Future of Nursing” report, the Robert Wood Johnson Foundation and the AARP Foundation created a Future of Nursing: Campaign for Action. Indiana is one of 15 states participating. IU’s Boland and Richard Kiovsky, executive director of the Indiana Area Health Education Center, are co-chairing that coalition.
Kiovsky said the biggest issue right now is figuring out how to use nurses within the health care system to create the greatest benefit for patients. The answer that appears to have the most momentum is the concept of interprofessional team care. He said a study of an intensive care unit that instituted team-based care found a 25-percent reduction in deaths compared with conventional ICUs.
“To get a 1 to 2 percent change with some sort of intervention is important,” Kiovsky said. “But to see that, it was significant.”
So while health care—and nursing in particular—faces multiple challenges, those involved are optimistic.
“I think that nursing has a critical place in leading and co-leading with our physician and administration colleagues and other health care providers to create the innovations that are going to be required to meet the demands of health care reform,” said Cindy Adams, chief nursing officer for Community Health Network. “It’s going to be a time for nursing to shine.”•
Please enable JavaScript to view this content.

Editor's note: You can comment on IBJ stories by signing in to your IBJ account. If you have not registered, please sign up for a free account now. Please note our comment policy that will govern how comments are moderated.