Subscriber Benefit
As a subscriber you can listen to articles at work, in the car, or while you work out. Subscribe NowIndianapolis-area hospitals have too many empty beds.
 That’s one reason Indiana University Health is working on plans to consolidate its University and Methodist hospitals.
That’s one reason Indiana University Health is working on plans to consolidate its University and Methodist hospitals.
It’s behind IU Health’s hospital in Martinsville studying whether it will offer inpatient services at all in the future.
It’s why Johnson Memorial Hospital in Franklin recently converted 25 patient rooms, which were used as recently as 2011, into offices for its billing staff.
And it’s a factor that essentially all Indianapolis-area hospitals will have to wrestle with as advances in non-invasive surgeries, changes in health care financing and now increasingly price-sensitive patients accelerate what has been a 40-year decline in the number of patients spending the night in hospitals.
“Most everybody who sees us does not see us in a hospital. That’s going to go down, down, down,” Community Health Network CEO Bryan Mills said during a February presentation to his employees.
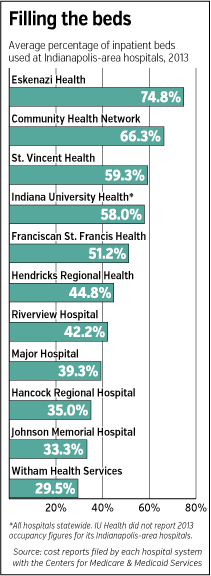
And Community’s Indianapolis-area hospitals have some of the highest occupancy rates among their peers—about 66 percent in 2013. The other large hospital systems had occupancy rates in the 50-percent range. County-owned hospitals in Indianapolis’ suburbs have occupancy rates ranging from 45 percent to as low as 30 percent.
Those rates have slipped slightly since 2011, even as hospitals reduce the number of beds they make available to patients.
“If you presume that technology will continue to improve and enhance and inpatient visits will continue to go downward—and I think that’s a fair assumption—that means the inpatient beds are going to go down,” said Ed Abel, a hospital accountant at Indianapolis-based Blue & Co. “Any facility that’s inside [Interstate] 465 is going to be reviewed at some point in time for its usefulness.”
He specifically mentioned Community East Hospital on Ritter Avenue and Community Westview Hospital on Guion Road.
Community East operates only 163 beds now—down from 800 beds three decades ago. But it keeps those beds about 70-percent full and has a bustling emergency room. Westview, by contrast, had occupancy of less than 40 percent last year, and has been losing money, according to people with knowledge of that hospital’s finances.
 Mills
MillsA Community spokeswoman declined to say whether Community was evaluating the future of its East and Westview hospitals. Mills has repeatedly said his hospital system is committed to keeping East open.
IU Health formed a committee in June to evaluate how best to merge Methodist and University hospitals into one location. That could mean either one or both of those facilities closes or is converted to another use.
IU Health’s downtown hospitals boast healthy occupancy rates of more than 70 percent. But with IU Health expecting inpatient use of hospitals to go down, the duplication of buildings and equipment—all of which sit just 1.5 miles apart—will become far harder to sustain financially.
IU Health doesn’t expect to see fewer patients. The aging baby boomers will almost certainly produce a surge in the need for medical care. But very little of that care will involve staying overnight in a hospital.
Even orthopedic surgeons are now starting to do joint replacement surgeries on an outpatient basis, and local health care experts expect local hospitals to start doing so as early as 2015.
That’s due partly to advances in technology. But it’s also due to changes coming from the federal Medicare program, which are often mimicked by private health insurers.
Medicare, the health plan for seniors, has launched a series of initiatives aimed at giving financial rewards to hospitals to cut out unnecessary surgeries, or to bill for them in a packaged rate, or to intervene with patients sooner so they never need expensive surgeries.
Those financing changes—which go by such names as accountable care, bundled payments and value-based contracts—have turned inpatient hospitals from places that could bring in lots of revenue to expensive assets whose use needs to be minimized.
Something similar happened 30 years ago, when Medicare adopted a new system of inpatient payment, known as Diagnosis Related Groups. That change helped cut in half the average length of stay in a hospital, from about nine days then to about 4.5 days now.
 Lauter
Lauter“The historical factors continue. We’ve just added on to that,” said Keith Lauter, chief financial officer at Franciscan St. Francis Health, which closed its Beech Grove hospital in 2012 after expanding its Indianapolis campus, which sat just seven miles away.
Lauter noted that Medicare now penalizes hospitals if they readmit too many patients within 30 days for the same conditions. And late last year, Medicare started requiring patients to stay over “two midnights” before it will pay the higher rates of an inpatient admission. The rule upped the incentive for hospitals to avoid short-term stays.
“We don’t see it as a temporary thing,” Lauter said. “We do see it as the new normal.”
The new normal is especially challenging for smaller hospitals, such as IU Health Morgan Hospital in Martinsville. It stopped delivering babies in February 2013. Around the state, there are 29 counties that have no inpatient obstetrical services, according to the Indiana Hospital Association.
IU Health Morgan is mulling a new model of care, which would likely focus on outpatient services, emergency care and medical transport when patients need more specialized care.
Similar hospitals are feeling the same pressures. In 2013, Johnson Memorial in Franklin had occupancy of 33.3 percent and Witham Health Services in Lebanon had 29.5 percent.
One thing that is keeping county-owned hospitals afloat is a recently discovered wrinkle in federal health care financing rules, which allows government agencies to draw down extra money for Medicaid patients. That program brought $313 million to Indiana hospitals and nursing homes last year.
 Heydon
HeydonCounty-owned hospitals also are finding savings where they can. This spring, Johnson Memorial moved 35 employees, primarily medical billing staff, into the inpatient hospital facility. It plans to demolish their old office space, which was in a separate, 35-year-old building.
Larry Heydon, CEO of Johnson Memorial, said he expects other hospitals to do more of the same, even making some cuts in medical care.
“They will not close their facility,” he said of county-owned hospitals. “But they will limit the services they provide.”•
Please enable JavaScript to view this content.

Editor's note: You can comment on IBJ stories by signing in to your IBJ account. If you have not registered, please sign up for a free account now. Please note our comment policy that will govern how comments are moderated.