Subscriber Benefit
As a subscriber you can listen to articles at work, in the car, or while you work out. Subscribe NowThe scribbling started in March 2010.
Immediately after the passage of the health care reform law that month, many employers scribbled back-of the-napkin calculations for how much they could save if they dropped health insurance coverage and instead paid the $2,000 per worker fine for doing so.
But the real scribbling is yet to come—and a lot more complicated. When health insurance exchanges start up in 2014, employers will actually have the option of turning those scribblings into action.
The question of the moment is, how many employers drop coverage? Several sophisticated studies by Rand Corp., the Congressional Budget Office and others have generally answered, not many. But last month, 30 percent of employers surveyed by McKinsey & Co. said they “definitely” or “probably” would drop coverage at some time after 2014.
So IBJ did its own back-of-the-napkin calculation, for an average small company paying average wages to its average-income family workers. What we found is this: Companies that drop insurance coverage could, without spending any more money than they are now, give workers an 11-percent raise or else help them save as much as $2,000 per year buying health coverage in one of the exchanges.
Employees buying single coverage would not fare as well, likely spending $1,000 more for health coverage in the exchanges compared with what they pay now through employer plans.
Those projections are based on numerous assumptions that could fail to prove out. And even if they do come about, employers could still shun the exchanges if employees perceive them as unattractive. The exchanges will be online marketplaces for health insurance, created and regulated by state governments or, if a state chooses, the federal government.
“Employers might drop coverage if health exchanges are up and operating successfully, if the company’s access to a healthy, productive work force is not adversely impaired, and if dropping employer-sponsored insurance does not put an employer at a competitive disadvantage to their direct competitors,” wrote Paul Keckley, executive director of the Deloitte Center for Health Solutions, in a June 27 report.
 Some observers, however, think financial straits will push employers—particularly small ones—to use the exchanges no matter what.
Some observers, however, think financial straits will push employers—particularly small ones—to use the exchanges no matter what.
“All I hear is, ‘I may have to, because there’s only so much that we can afford to do,’” said Barbara Quandt, Indiana director of the National Federation of Independent Businesses. “They’re all thinking about what they’re going to do.”
Employer reactions to the exchanges will be key for the success or failure of health care reform. If too many employers drop their plans and send workers to the exchanges, it could cause the federal government to pay far more in subsidies than it expects, exploding the costs of the exchanges.
Conversely, if no employers participate in the exchanges, it could thwart one of the law’s main mechanisms for expanding the number of insured Americans.
The health care reform law raises various taxes to help fund subsidies for low- and middle-income Americans to buy private health insurance policies through state-based exchanges. Private insurers will have to craft plans according to numerous rules in the new law, which aim to make the plans comparable from one insurer to another.
Those exchanges are scheduled to begin operating on Jan. 1, 2014. On that same date, all employers will be required to offer health insurance to their workers—or else pay fines—and all Americans will be required to have health insurance, or else pay a fine.
Of course, that last element of the law has sparked lawsuits by more than 20 states, which are wending their way through the federal courts on their way to the U.S. Supreme Court. So the entire law could be nullified.
Also, Republicans in Congress have vowed to repeal the entire law—and might have a shot at doing so in early 2013 if they gain control of the White House and U.S. Senate in the 2012 elections.
That has many employers doing nothing but casual analyses of the options they could pursue come 2014.
“There’s a little bit of a wait-and-see attitude to see what the courts and Congress do,” said Tom Easterday, executive vice president at Subaru of Indiana Automotive in Lafayette.
His company, which covers 7,000 people in its self-funded health plan, did a quick calculation in 2010 just to see how much it could save by dropping health coverage and paying the $2,000 per-worker fine—even though it had no intention of doing so. The answer: $20 million per year.
Many other firms did the same math, said Chris Sears, an employer benefits attorney at Ice Miller LLP.
“But the truth is, it’s not that simple,” Sears said. “In any remotely competitive [employment] environment, I’m going to have to pay something extra to my employees so they can get [health coverage] elsewhere.”
And once an employer starts raising workers’ pay (as opposed to health benefits, which are tax-free), they’ll also have to pay more in payroll taxes and retirement plan contributions and unemployment insurance and other benefits that are based on income. And the workers will face more in taxes, too, which dampen the savings from dropping coverage.
It also makes the math on these calculations really messy.
IBJ did the messy math, below, for a fictional 100-person firm, paying small-company wages and small-company benefits. IBJ also did the messy math from an average worker’s standpoint, someone making about $45,000 a year, with a spouse and two kids.
What follows is a discussion of those math calculations and the choices employers and workers will face along the way.
Average Small Co.
For this exercise, the average small company pays all 100 of its workers yearly wages (including any bonuses, overtime, etc.) of $45,000, which is a tick higher than the average pay reported by the U.S. Bureau of Labor Statistics.
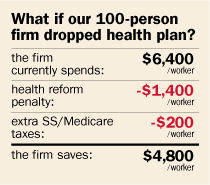 The management of this company decides it will drop coverage and compensate employees in other ways—as long as doing so allows it to spend no extra amount of money.
The management of this company decides it will drop coverage and compensate employees in other ways—as long as doing so allows it to spend no extra amount of money.
The advantage of that action would be to get control over health insurance premiums—which grow each year 5 percent to 7 percent—but sometimes leap by up to 40 percent.
The managers of this firm reason that if they could grow health benefit spending along with wages, which have been rising 2 percent to 3 percent annually, they’ll save in the long run.
That’s the thinking of Mark Messmer, vice president of Messmer Mechanical Inc., a heating and cooling contractor in Jasper. With 49 employees, Messmer is not currently subject to the $2,000 per-worker fines, but if it added just one more worker—even a part-timer—it would be.
“We’d say, ‘Here’s what we were paying in your insurance. We’re going to make a one-time adjustment in your salary,’” said Messmer, who is also in his second term as a Republican state representative. “And then send them off to the exchanges.”
Such an assumption may prove rosy, noted Chris Sears, an employee benefits attorney at Ice Miller LLP, if employees find that contributions from their employer buy them less and less each year.
But Messmer—after his company sustained health insurance premium hikes of 25 percent, 30 percent and 44 percent the past three years—figures many employers would do the exact same thing regardless.
“At what point do I throw up my hands and say, ‘I’ll pay the $2,000 fine just to survive?’” he said. “I would be stunned in our size of business, if 100 percent of them don’t drop coverage.”
Each year, the Average Small Co. is spending $6,400 per worker on a family health insurance plan, according to data from BLS and the California-based Kaiser Family Foundation. Employers pay about twice as much for family policies as they do for single coverage.
For employers with more than 50 workers, dropping coverage would prompt a $2,000 federal fine—for each worker over the number 30.
So for Average Small Co., it pays a fine on only 70 of its 100 workers, for a total cost of $140,000—or an average of $1,400 per worker.
Even after the fine, the company would pay $5,000 less per worker than it’s paying now—money the company can give directly to its employees to help them buy health insurance. But before it pays that money, it must consider that the new compensation will be subject to Social Security and Medicare taxes—of 7.5 percent—which it avoided when spending that money directly on health care benefits.
Those taxes hack $200 per worker off the money the employer can give, reducing the total to $4,800 per worker.
 If given to every worker evenly, that money would constitute an 11-percent raise for the average-pay worker. Of course, after taxes—local, state and federal income taxes, as well as Social Security, Medicare and unemployment taxes—the raise is less. With the taxes and other things that are based on income, like Worker’s Compensation, disability and life insurance premiums and also any income-based retirement contributions—the average worker takes home just $3,100 extra.
If given to every worker evenly, that money would constitute an 11-percent raise for the average-pay worker. Of course, after taxes—local, state and federal income taxes, as well as Social Security, Medicare and unemployment taxes—the raise is less. With the taxes and other things that are based on income, like Worker’s Compensation, disability and life insurance premiums and also any income-based retirement contributions—the average worker takes home just $3,100 extra.
McKinsey & Co. analysts contend that the extra cash might be perfectly satisfactory to most workers. Its consumer research has found that 85 percent of workers would remain with an employer that dropped health coverage, and that employees value cash compensation several times more than health benefits.
But Tom Easterday, executive vice president at Subaru of Indiana Automotive, finds that idea problematic. Employers do have an interest in healthy employees—to cut down on absenteeism and to improve productivity. So he thinks it’s more likely employers would place money in some sort of savings vehicle, like a health savings account or a health reimbursement account.
“The danger that a lot of companies would see, in terms of giving it as salary, is you could still end up with an employee that doesn’t have health care coverage,” Easterday said. “I don’t think any employer wants to have an employee go uninsured.”
Following that logic, Average Small Co. decides to help employees avoid the hefty tax bite the extra income would cause by plunking the money instead into health reimbursement arrangements. That way, the company avoids that extra $200 per worker in payroll taxes and the employees can use the money tax free to purchase insurance or to pay for medical care directly.
But rather than giving each employee the same amount of money, Average Small Co. decides to follow its current policy on health insurance: pay twice as much for the half of its work force buying family health insurance as it does for the half buying single coverage.
So instead of giving $5,000 equally to all workers, Average Small Co. instead gives $6,700 to family-policy workers and $3,300 to single-policy workers.
Pat the Average Worker
Pat the Average Worker makes average money for an employee of a 100-person firm and buys health insurance that also covers a spouse and two kids.
 The average small-business worker buying a family policy already contributes $4,700 per year toward the cost of an employer-sponsored health plan, according to an employer survey by Kaiser Family Foundation. Because it’s applied to an employer plan, that money is not taxed.
The average small-business worker buying a family policy already contributes $4,700 per year toward the cost of an employer-sponsored health plan, according to an employer survey by Kaiser Family Foundation. Because it’s applied to an employer plan, that money is not taxed.
Once the employer stopped offering coverage, the money would be taxed, whittling down the worker’s contributions to just $3,100.
So, combined with the $6,700 given by Average Small Co., Pat the Average Worker has $9,800 to spend on health insurance in the health insurance exchange.
Pat the Average Worker earns $45,000 per year. But the household income for Pat the Average Worker is $70,000, according to Census Bureau data. This income is equal to 313 percent of the federal poverty limit, which qualifies Pat’s family for about a $5,000 subsidy in the health insurance exchange.
According to projections by the Kaiser Family Foundation, based on data from the Congressional Budget Office, the average family policy in the exchange—after the subsidy—will cost $6,500 in today’s dollars.
So Pat the Average Worker could buy the $6,500 policy and still have $3,300 left over.
The exchange plan will come with a $3,000 deductible, according to three estimates conducted by benefits and actuarial firms, in another study commissioned by Kaiser. Currently, Average Small Co. has a $1,700 deductible on the plan it provides Pat the Average Worker, which is consistent with Kaiser data.
So, assuming Pat the Average Worker maxes out the deductible each year, it would cost $1,300 more than Pat is currently paying. Therefore, Pat saves $2,000 overall.
Is that enough savings to make the exchanges the attractive option for employers? Probably not all by itself.
McKinsey & Co. analysts projected that employers would probably still need to supplement their contributions toward health insurance with other help, such as benefits brokers to guide workers through exchanges or wellness programs.
But the attractiveness of giving raises or achieving savings in the exchanges or simply ending the outsized premium increases is likely to be enough to make employers investigate the possibility, said Kevin Woodhouse, a health care attorney at Ice Miller LLP.
“Everybody,” he said, “is going to have to look at it.”•
Please enable JavaScript to view this content.

Editor's note: You can comment on IBJ stories by signing in to your IBJ account. If you have not registered, please sign up for a free account now. Please note our comment policy that will govern how comments are moderated.