
Health insurance premiums poised to spike over drug costs, tariff threats
In explaining the rising prices, insurers and employers point to two recent factors: the tariffs on pharmaceutical imports and the high cost of new obesity treatments.

In explaining the rising prices, insurers and employers point to two recent factors: the tariffs on pharmaceutical imports and the high cost of new obesity treatments.

Planned Parenthood said Thursday’s ruling means that more than 1.1 million patients can’t use their Medicaid insurance at its health centers.

President Donald Trump signed a memo Tuesday that directs the FDA and other agencies to step up enforcement against ubiquitous prescription drug ads on TV, websites and social media.
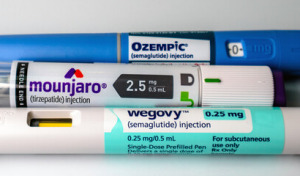
The restructuring, which would eliminate 11% of the company’s workforce, aimed to reduce organizational complexity and speed up decision-making as the company faces a more competitive market for obesity drugs.

The threat comes as Trump also pressures drugmakers to lower prices of pharmaceuticals in the United States.

SIHO Insurance Services is tackling the gargantuan challenge of growth in the employer-based benefits market in Indianapolis and across the state.
Indiana ranks 11th among the states in terms of the percentage of population with medical debt in collections, one survey shows.

The revamped vaccines target a newer version of the continuously evolving virus and are set to begin shipping soon.

The company’s shares rose as much as 4.3% Tuesday after Eli Lilly announced the trial results for orforglipron.

Price increases could be especially stark in individual coverage marketplaces, where insurers also are predicting the federal government will end some support that helps people buy coverage.

Testimony on Monday set the stage for an interim committee to find a balance between growing medical debt weighing down Hoosiers and allowing health care providers to collect what’s owed.

Health Secretary Robert F. Kennedy Jr. announced Tuesday that 22 projects, totaling $500 million, to develop vaccines using mRNA technology will be halted.

Hair loss isn’t new. What’s different today, experts say, is that male anguish about it has never been more evident. Social media, dating apps, “Zoom dysphoria” and a sometimes predatory marketplace are stoking the anxiety.

Trump administration officials have offered mixed messages about GLP-1s and whether they should be relied upon for weight loss by obese and overweight Americans.

Parkview said the hospital would be roughly 200,000 square feet, accommodate up to 40 inpatient beds and offer a 24/7 emergency department.

The new program is expected to allow Americans to share personal health data and medical records across health systems and apps run by private tech companies, making it easier to access health records and monitor wellness.

Fort Wayne-based hospital system Parkview Health does not have a hospital in the Indianapolis area, but it is seeking to increase its name recognition in the state’s political center and largest market.

In its lawsuit, Planned Parenthood had argued that it would be at risk of closing nearly 200 clinics in 24 states if it were cut off from Medicaid funds.

Attorney General Todd Rokita announced Monday that Indiana is expected to receive another $16.5 million as part of the latest multistate opioid settlement.

The company’s UnitedHealthcare business covers more than 8 million people as the nation’s largest provider of Medicare Advantage plans.